Hits: 152
 |
Enjoying this newsletter? Why not share it with a friend?
The opioid crisis, rural health, and other stark realities
What this “coastal elite” learned at the country’s biggest drug conference
|
|
|
|||||||||||||||
I’ll admit the label.
I grew up in a small Northern California town, but I’ve spent most of my adult life in places people mean when they say “coastal elite.” The Bay Area, San Diego, and now New York City, where I’ve been writing a public health newsletter for the past two years about topics like vaccine uptake, fluoride debate, and harm reduction programs. All things I care about and know about.
Last week, I was in a Nashville hotel lobby with that familiar conference energy: lanyards, coffee cups, and people craning to read each other’s name tags. I was there for the RX Summit, the country’s largest annual meeting on substance use and addiction, and I’d spent the morning watching sessions about fentanyl test strips and naloxone distribution.
Then I sat down across from a man from eastern Kentucky, and my frame of reference completely flipped on its head.
He grew up there, is in recovery himself, and now devotes his time to doing outreach with kids across his county. Playing basketball with them and showing up every single week as a trusted adult that a lot of them don’t have at home.
More than 60% of the kids in his county don’t live with a parent. He explained how substance use, incarceration, and poverty created ripple effects in a crisis that has been rewriting family structure for a generation.
I write about public health for a living, but I was speechless. All of a sudden, my usual public health lens (“talk to your doctor,” “get screened,” “get vaccinated”) felt so…out of touch.
He wasn’t the only one who shifted my thinking.
I talked to people from northeastern Tennessee who are scared to drink their tap water.
I heard story after story from clinicians and community workers about what it means when the nearest treatment center is two hours away.
I met people in recovery who had rebuilt their lives against all odds and are now thriving with families.
I walked away from that conference with three lessons I can’t stop thinking about, and that I hope to apply to this newsletter.
1. Public health priorities look different when basic access is broken
What stayed with me was the word he used for what he does: prevention.
In the world I write from, prevention means vaccination, screening programs, and public awareness campaigns. Where he works, it means being the adult who shows up to play basketball because the other adults are gone. Same word, but with a completely different world underneath.
The PFAS situation in northeastern Tennessee made this even clearer.
People there described being afraid to drink from their own taps, and that fear is grounded in real data: the Sierra Club found that 60% of surface waters in the region were contaminated, and state testing has detected PFAS in several raw waterways supplying public drinking water.
It’s a concern in New York, too, where some counties now offer free PFAS testing for private well water.
But when the baseline question in a community is whether the water coming out of the tap is safe at all, debates about fluoride additives don’t just feel like a lower priority. They feel like they’re arriving from a different conversation entirely—one happening somewhere far away, about problems these communities don’t even have the luxury to think about.
Public health isn’t one single issue. It can look very different depending on your community, your resources, and what problems are most urgent.
2. “Prevention” assumes infrastructure that many Americans don’t have
We are at a critical point for rural health care as clinics across the country close at high rates. Medicaid makes up 40% of hospital revenue in some rural regions.
In the Adirondacks, 28% of residents rely on it, as do half of all births and two thirds of nursing home residents. Many people there have seasonal or part-time work that doesn’t come with employer health insurance. Nearly a third of rural hospitals in New York state are already at immediate risk of closure, and that was before the most recent round of proposed Medicaid cuts.
What this means in practice is driving two hours, or more, for buprenorphine (a treatment for opioid dependence), skipping the prenatal appointment because there’s no one to cover your shift and the clinic is that far away, deciding whether a child’s injury is bad enough to justify a trip to an emergency room two counties over. Community workers I met at this conference drive hours to deliver naloxone, and recovery coaches are working out of church basements and school gyms.
Many are navigating a health care system that looks almost nothing like it does for the coastal elite.
There’s a gap between the public health guidance produced and what’s actually possible for the people receiving it.
3. Hope comes from understanding that public health is a team sport
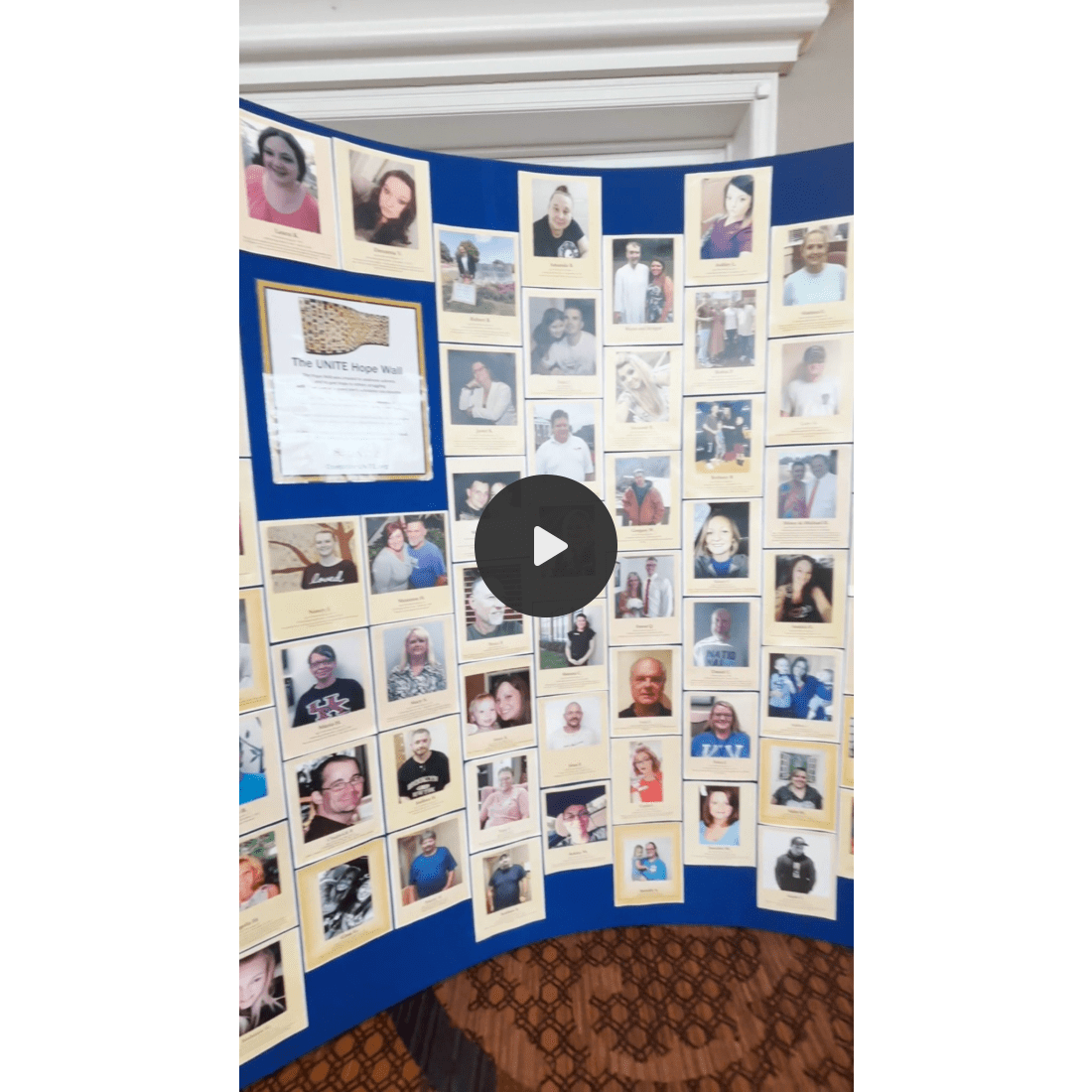
In the lobby was something called a “Hope Wall.” It was covered in photographs and stories of people in active recovery, faces and names attached to the statistics I spend my time writing about. Some with kids, dogs, and friends. I’ve never stood in front of something like that at a conference before, and had to take a breath before moving on.
The Operation UNITE Hope Wall. Song: Here Comes The Sun Instrumental by Emerald Empire Band.
The people I met last week weren’t waiting for better systems or more political will before showing up.
They were already there, at churches, knocking on doors, on county basketball courts, showing up with whatever they had. It’s a reminder of what this work is actually anchored in: people, families, and communities that deserve better than what they’ve got. And that’s what we’re all working towards.
Bottom line
For this city girl, spending time at the summit was both humbling and inspiring. It was a reset. A reminder to get out of my bubble, to listen more, and to make sure this work stays grounded in real lives. I hope I can bring that to this newsletter, but I’ll need your help learning more about your experiences, your questions, and your realities.
The man I met in that lobby is still showing up to play basketball with kids who need him. That’s public health, too. I want to remember that.
Love,
Your NY Epi
Dr. Marisa Donnelly, PhD, is an epidemiologist, science communicator, and public health expert. This newsletter exists to translate complex public health data into actionable insights, empowering New Yorkers to make informed and evidence-based health decisions.
Thanks for your financial support of Your Local Epidemiologist in New York! I couldn’t do this without you. — Marisa