Hits: 217

The dreaded and much anticipated triple-demic is finally here—for the first time RSV, flu, and COVID-19 are rising together. And it’s not looking pretty. Here is the current state of affairs.
Overall
Last Friday Twitter covered my reaction to the latest data pretty clearly: Holy crap. There are a lot of sick people in the United States right now.

(Source: CDC)
This level is truly unprecedented; we’ve never seen such high levels of ILI activity at this time of year. The map above is typically green (see below for this time in previous years). In fact, notice that before 2019, we didn’t even have the dark red/purple colors.

ILI Map by Year (Source: CDC) Note: You will notice that 2020-2021 are very green (although COVID-19 was high). There are many epidemiological reasons for this, including people avoiding doctors offices at the time.
Yesterday, the CDC Director said: “hospitalizations are the highest now than they have been in the past decade.” This is truly concerning given a backdrop of burnt out healthcare workers and low staff levels.

While ILI surveillance gives us a picture of symptoms overall, we do have some (imperfect) surveillance for specific diseases.
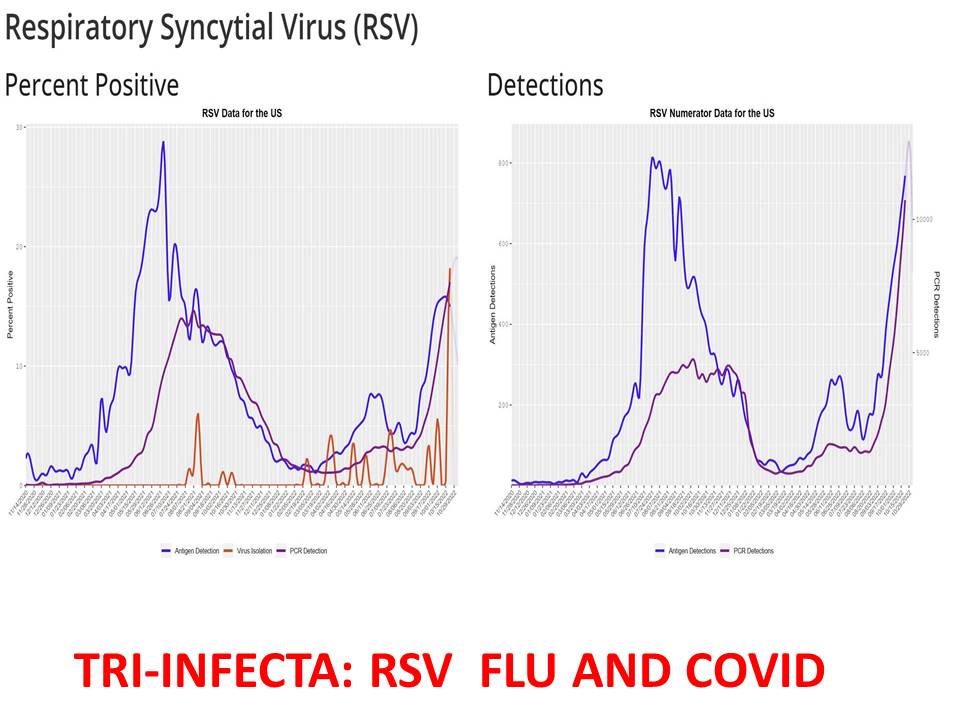
RSV
RSV continues to rise. We may be seeing the first signs of peaking on a national level (bottom right graph). This is expected given that test positivity rates have already clearly peaked (bottom left graph). There are certainly regional differences, as the South has clearly peaked (at least so far—Thanksgiving activity may change this) and West hasn’t slowed down yet.
U.S. RSV positivity rates and cases (Source: CDC)

Flu
Flu cases are increasing and increasing fast. Flu hospitalizations are lagged (much like COVID-19) but increasing. Flu season outbreaks typically start in schools (hitting healthy children). Then the virus takes time to get to older adults. We expect hospitalizations to continue to rise in weeks to come.

In Canada, hospitalizations by age are clearly tracked. The highest risk for hospitalization is in those under 4 years old and those over 65 years. This likely reflects U.S. patterns, too.

Influenza related hospitalizations in Canada, by age group. Source here.
As Inside Medicine reported, for the first time during the pandemic, flu hospitalizations overtook COVID-19 hospitalizations last week. This may be a one-off occurrence since COVID-19 hospitalizations are increasing now, too, but it is noteworthy.
Image: Benjy Renton for Inside Medicine. Source here.
We don’t know if this will be the “worst flu season we’ve ever seen.” The Southern Hemisphere (Australia specifically) had a high number of flu cases but moderate levels of hospitalizations. Epidemiologists are crossing our fingers that this is what the Northern Hemisphere will see, too.
COVID-19
COVID-19 is on the rise across the globe due to the combination of seasonal changes, behaviors changes, and the variant soup. In the U.S., all signs point to the beginning of a wave. For example, SARS-CoV-2 in wastewater is rapidly increasing across all regions.
SARS-CoV-2 National Wastewater Trends, over time. Dark blue= wastewater; Light blue/green= Reported cases (Source: Biobot Analytics)
One major concern is the rapid rise in hospitalizations among older adults, which has exponentially increased 28% in the past two weeks. In many states, like California, the rate of hospitalizations is higher than the BA.5 wave, BA.2 wave, and/or Delta wave.

New Hospital Admissions, over time (CDC)
This is partly (or wholly) due to abysmal vaccination rates—only 1 in 3 adults over the age of 65+ have their fall COVID-19 booster. A public health failure. Without a recent booster, many people are technically vaccinated but not protected. I appreciated a recent U.K. public health campaign displaying the best messaging I’ve seen thus far.

(Source: Sean Kennedy)
Thanksgiving was 1.5 weeks ago, and because of it, many social networks expanded, providing new opportunities for viruses to spread. For COVID-19, it takes about ~2 weeks to see the epidemiological impact of holidays. The recent COVID-19 uptick may be partially explained by a “Thanksgiving effect,” although we are seeing an uptick in other countries that don’t celebrate Thanksgiving.
I expect Thanksgiving will springboard us into more RSV and flu, too, but this surveillance is delayed.
Bottom line
This viral season is like no other. I’m running out of adjectives to describe it. (Unprecedented. Worrisome. A pain. Exhausting.)
Unfortunately, we don’t know how long this will last or how bad it will get. I’m especially concerned for hospital systems, kids under 5, and adults over the age of 65, as they are at highest risk.
There’s a lot we can do: mask, test before seeing loved ones, get that airflow moving, stay home when you’re sick.
The least you can do for a healthy season is get a flu and fall COVID-19 booster. If you haven’t gotten one yet, it’s never too late.
